The Critical Link Between Testosterone and Sleep Apnea

The connection between testosterone and sleep apnea is a tricky one. It's a genuine two-way street where one problem can directly cause or worsen the other. Untreated obstructive sleep apnea (OSA) is known to crush your body's natural testosterone production. On the flip side, starting testosterone replacement therapy (TRT) can sometimes unmask or even aggravate a case of sleep apnea you didn't know you had.
The Hidden Connection Between Hormones and Sleep

If you're constantly exhausted, dragging yourself through the day even after a full eight hours in bed, you might be trapped in a frustrating cycle. The link between your hormones and sleep quality is far more intimate than most people realize, creating a feedback loop that's tough to escape without understanding what's really going on.
This isn't just a simple case of one thing leading to another. Instead, it’s a dynamic where each condition can feed the other, making both worse over time. Getting a handle on this relationship is the first step to finally getting your energy back.
The Vicious Cycle Explained
Imagine your body's hormone production is a high-tech factory that runs the night shift. Obstructive sleep apnea is like a rogue saboteur who keeps flipping the main breaker, shutting down the entire assembly line just when it’s supposed to be most productive.
These constant interruptions don't just happen without consequences. They kick off a self-perpetuating cycle of fatigue and hormonal chaos. Here’s a play-by-play of how it works:
- Sleep Apnea Kills Hormone Production: Your body manufactures the vast majority of its testosterone during deep, restorative sleep. OSA shatters this crucial process with frequent awakenings and oxygen drops, essentially sending an emergency signal to your brain to stop making testosterone.
- Low Testosterone Can Make Apnea Worse: As testosterone levels fall, men often experience an increase in body fat and a decrease in muscle tone. This is a bad combination for sleep apnea. Extra fat around the neck physically narrows your airway, and weaker throat muscles are more prone to collapsing during sleep, causing an obstruction.
- Symptoms Overlap and Get Worse: The classic signs of both conditions are nearly identical: daytime fatigue, brain fog, and a nonexistent libido. When you're dealing with both, these symptoms can become overwhelming, making it nearly impossible to exercise or stick to a healthy diet, which in turn worsens both the apnea and the hormone imbalance.
This damaging cycle means that trying to fix one issue without addressing the other is often a losing battle. Treating low testosterone without diagnosing underlying sleep apnea can be risky, while ignoring low T levels can make managing OSA much more difficult.
To give you a quick overview, here’s how the two conditions influence each other:
Testosterone and Sleep Apnea Key Interactions at a Glance
| Interaction Pathway | Impact of Sleep Apnea on Testosterone | Impact of Testosterone Therapy on Sleep Apnea |
|---|---|---|
| Hormone Production | Repeated sleep fragmentation and low oxygen levels during the night directly inhibit the body's natural production of testosterone. | Exogenous testosterone doesn't directly cause OSA but can worsen it in susceptible men, potentially by affecting airway muscle control or fluid retention. |
| Body Composition | Contributes to fatigue and metabolic changes that favor fat gain and muscle loss, common risk factors for low testosterone. | TRT helps build muscle mass and reduce fat, which can be beneficial. However, initial changes might affect airway dynamics. |
| Symptom Overlap | Causes daytime fatigue, low libido, and mood swings, which are often mistakenly attributed solely to "low T." | Can improve energy and libido, but if OSA is the root cause, these benefits may be limited or mask the underlying sleep disorder. |
This table highlights why a comprehensive approach is so crucial. You have to look at the full picture.
Why This Connection Matters for You
Navigating the world of testosterone and sleep apnea demands a smart, careful approach. If you're a man experiencing the classic symptoms of low T—fatigue, weight gain, moodiness—it's vital to consider that a sleep disorder might be the real culprit. In fact, a huge number of men diagnosed with OSA are also found to have clinically low testosterone levels.
Likewise, for anyone considering or already on TRT, understanding how it might affect your breathing during sleep is non-negotiable. Any responsible doctor will now screen for sleep apnea before starting testosterone therapy. It's a critical safety step to make sure the treatment is both safe and effective. This guide will give you the clarity you need to tackle both conditions, break the cycle, and get on the path to better health.
How Sleep Apnea Suppresses Your Testosterone Production

To really get how obstructive sleep apnea (OSA) torpedoes your testosterone, picture your body as a sophisticated factory that runs its most important assembly lines during the night shift. For men, that overnight work includes churning out the majority of their daily testosterone. This whole process is precision-timed and absolutely depends on getting deep, uninterrupted sleep.
OSA is like a saboteur cutting the power to the factory floor over and over again. Every time you stop breathing—an event called an apnea—your brain senses the emergency and jolts you partially awake just enough to restart your breathing. You probably won't even remember these arousals, but they happen repeatedly, shattering your deep sleep cycles and bringing that critical hormone production to a grinding halt.
This isn't a minor hiccup. It's a fundamental breakdown of your body's endocrine system. The link between testosterone and sleep apnea isn't some coincidence; it's a direct physiological consequence of being starved of quality sleep.
The Breakdown of the Hormone Assembly Line
The hormonal damage from OSA unfolds through two primary mechanisms that team up to tell your testes to shut down testosterone production. When your factory's assembly line is constantly being stopped and restarted all night long, the whole operation becomes inefficient and chaotic.
First, you have the repeated nosedives in your blood oxygen levels, a state known as hypoxia. This oxygen deprivation is a massive stressor, sounding an alarm that forces your body into survival mode. When your body is just trying to survive, non-essential tasks like making hormones get pushed to the back burner.
Second, there are the frequent awakenings. Even if they're just micro-arousals you don't recall, they cause what experts call sleep fragmentation. Your body simply never gets to spend enough consecutive time in the deep, restorative stages of sleep where the bulk of testosterone is actually made.
Together, these two factors create a perfect storm—a hostile environment where hormone production can't possibly thrive.
The Role of Stress Hormones and Inflammation
When your body is dealing with the dual threats of low oxygen and fragmented sleep, it shifts into a state of high alert. This triggers the release of stress hormones, especially cortisol. Think of cortisol and testosterone as being on a seesaw; when one goes up, the other tends to go down. The chronic nightly surges in cortisol from untreated OSA directly suppress the signals from your brain that tell the testes to get to work.
On top of that, this constant state of emergency leads to systemic inflammation throughout your body. Chronic inflammation is another powerful inhibitor of testosterone synthesis, further compromising your hormonal health. Night after night, this battle leaves your body too stressed and inflamed to maintain healthy testosterone levels.
The research on this is pretty conclusive. A major 2021 meta-analysis looked at 18 different studies involving over 1,800 men and confirmed a powerful inverse link. Men with OSA had significantly lower testosterone, and the problem got dramatically worse as the severity of the sleep apnea increased. You can read the full research about these findings here.
The takeaway is clear: Untreated sleep apnea doesn't just make you tired. It actively dismantles your body's ability to produce one of its most important hormones by creating a perfect storm of stress, oxygen deprivation, and inflammation.
Recognizing the Impact on Your Health
This whole process explains why so many men who show up with classic low T symptoms—fatigue, low libido, weight gain, and brain fog—might actually be suffering from an undiagnosed but highly treatable sleep disorder. The symptoms you're chalking up to just "getting older" could be direct results of your body not getting the oxygen and restorative sleep it desperately needs.
Understanding that OSA is actively sabotaging your body's testosterone factory makes it clear why just treating the low T without addressing the sleep apnea is often an incomplete—and potentially risky—solution. The first real step toward restoring your hormonal balance is to fix the nightly disruptions that are causing the problem in the first place.
Can Testosterone Therapy Worsen Sleep Apnea?
This is probably the number one concern for men thinking about Testosterone Replacement Therapy (TRT), and it's a completely fair question. The short answer is no, TRT does not cause sleep apnea out of the blue in a healthy person.
However, it can absolutely act like an amplifier. If you have a mild or undiagnosed case of obstructive sleep apnea (OSA) lurking beneath the surface, TRT can turn up the volume on the problem.
Imagine your airway is a hallway you walk through every night during sleep. For someone with mild OSA, the walls of that hallway are already a bit too close for comfort. Starting TRT doesn't build new walls, but it can subtly make the existing ones a little thicker or less stable. That increases the chances they’ll collapse and block your airflow.
The connection between testosterone and sleep apnea isn't random; it's tied to a few specific physiological mechanisms. Once you understand them, the fear starts to fade, replaced by a clear, manageable plan for moving forward safely.
How Testosterone Can Affect Your Airway
The idea that testosterone might make sleep apnea worse isn't just a guess. It’s based on how the hormone actually works in your body. While some early studies caused a bit of a stir, modern research and clinical experience show a different picture: with proper screening and medically supervised dosing, these effects are usually minimal and easy to manage.
There are two main ways testosterone can influence your breathing while you sleep:
- Changes in Upper Airway Muscles: Testosterone is a key player in muscle tone and function. One leading theory is that introducing testosterone from an outside source can change the "stiffness" of the muscles that hold your throat open. If they become too relaxed or less responsive, they're more likely to collapse during sleep.
- Fluid Retention: It's pretty common to retain a bit of extra fluid when first starting TRT. If that fluid settles in the soft tissues of your neck, it can physically narrow your airway—similar to what happens when you gain weight in that area. The good news is this effect is often temporary and fades as your body gets used to the new hormone levels.
It’s crucial to remember that these changes don't happen to everyone. If you have a wide-open airway and no other risk factors, these small shifts probably won't cause any trouble. But for someone already on the verge of developing OSA, it can be just enough to tip them over the edge.
The Real-World Risk Data
So, what does the research actually say? A major retrospective study that tracked 6,405 men on TRT gives us a much clearer picture. It found that about 14% were diagnosed with OSA within two years of starting therapy.
That might sound high, but it was only slightly more than the 12% baseline rate found in men with low testosterone who weren't on TRT. This suggests the increased risk is nuanced, not dramatic. The key finding, however, was that factors like obesity, a family history of OSA, and alcohol use significantly amplified this risk. You can discover more insights about these findings on auajournals.org.
This data reinforces a critical point: TRT isn’t the bad guy here, but it demands respect. The therapy works within the context of your overall health. A smart, responsible approach means identifying and managing underlying risks before they become a problem.
This is exactly why screening for sleep apnea has become a non-negotiable first step in any modern, reputable hormone therapy protocol.
Why Screening Before TRT Is Essential
Knowing that TRT can potentially make an undiagnosed breathing issue worse, proactive screening is your best line of defense. Any responsible clinician will assess your risk for sleep apnea before even thinking about writing a prescription.
This isn't meant to be a roadblock. It's a safety measure to ensure you get all the incredible benefits of TRT without sacrificing your sleep quality or your health.
This approach empowers you to start therapy with confidence, knowing every variable is being watched and managed. By addressing any potential sleep breathing issues upfront, you create a much safer and more effective path to getting your hormones, and your life, back in balance. To learn more about what to expect, check out our guide on the pros and cons of Testosterone Replacement Therapy.
Decoding Your Symptoms: Low T and OSA Overlap
One of the trickiest parts of the testosterone and sleep apnea connection is just how much their symptoms mirror each other. If you're wrestling with crushing fatigue, persistent brain fog, and zero motivation, it’s all too easy to assume you know the cause. Is it low testosterone? Is it a sleep disorder? The reality is, telling them apart based on how you feel is nearly impossible.
This is precisely why trying to diagnose yourself is a bad idea. You could end up treating the wrong problem while the real culprit—or a second co-existing condition—is left to cause more issues. It's a frustrating cycle that keeps you from ever feeling your best.
It's like trying to solve a puzzle where the pieces seem to fit in several different spots. That feeling of being completely wiped out during the day? That’s a classic sign of both low T and OSA. Same goes for a tanked libido, unpredictable mood swings, and finding it hard to focus. You could have any of these and be dead sure it's one thing when it's actually the other, or even both.
The Great Symptom Overlap
While a lot of the signs look identical, a few subtle differences can sometimes point you in the right direction. Just remember, these are simply clues, not a diagnosis. The real goal is to see just how tangled this web can be and why getting a professional opinion is so critical.
Some symptoms do lean more heavily toward one condition. For instance:
- Morning Headaches: Waking up with a throbbing headache is a tell-tale sign of OSA, often caused by a buildup of carbon dioxide in your blood from not breathing properly all night.
- Loss of Muscle Mass: If you feel like you're losing strength and your muscles are shrinking despite working out, that points more directly toward a hormonal problem like low testosterone.
- Observed Apneas: This is the most direct clue. If a partner or family member tells you that you stop breathing, snore like a freight train, or gasp for air while you sleep, that’s a huge red flag for sleep apnea.
But even with these distinctions, the shared symptoms are what cause the most confusion. Trying to figure it out on your own can lead you down the wrong path, wasting your time and money while you continue to feel awful.
Symptom Checker: Low Testosterone vs. Sleep Apnea
Trying to make sense of this confusing picture can be tough. The table below helps break down which symptoms tend to align with which condition. Pay close attention to how many fall into the "Significant Overlap" column—this is where the real diagnostic challenge lies.
| Symptom | Commonly Associated with Low Testosterone | Commonly Associated with Sleep Apnea | Significant Overlap |
|---|---|---|---|
| Fatigue | General lack of energy, feeling drained. | Severe daytime sleepiness, feeling unrefreshed. | ✔️ |
| Low Libido | Decreased interest in sex. | Often a side effect of fatigue and poor sleep. | ✔️ |
| Mood Changes | Irritability, depression, and mood swings. | Irritability and moodiness from sleep deprivation. | ✔️ |
| Weight Gain | Increased body fat, especially around the belly. | Often both a contributing factor and a symptom. | ✔️ |
| Poor Focus | Difficulty concentrating, "brain fog." | Memory problems and poor mental clarity. | ✔️ |
| Loud Snoring | Not a direct symptom. | A hallmark sign of an obstructed airway. | |
| Muscle Loss | Noticeable decrease in strength and mass. | Not a primary symptom. | |
| Morning Headaches | Not a typical symptom. | A very common sign of OSA. |
This comparison makes it crystal clear why a professional evaluation is non-negotiable. Even if you're experiencing symptoms that scream low T, like a loss of muscle, a clinician needs to dig deeper to understand your true risk for testosterone and sleep apnea. They have the right screening tools and lab tests to pinpoint the real source of your issues and build a plan that actually works.
To get a better handle on the hormonal side of the equation, you can learn more about identifying low free testosterone in our comprehensive guide.
A Proactive Guide to Managing OSA and TRT Safely
When we talk about testosterone and sleep apnea, the approach has to be safety-first. Starting Testosterone Replacement Therapy (TRT) is about so much more than just raising your T levels—it's about getting your entire system back online and feeling your best. But if an undiagnosed sleep disorder is lurking in the background, it can sabotage your progress and even introduce new health risks.
This isn't about putting up roadblocks to getting treatment. Think of it as a clear, common-sense roadmap that any experienced clinician will follow to make sure your journey with TRT is both safe and effective. By sorting out your sleep quality from the very beginning, you’re laying the foundation for better results with fewer complications down the line.
The whole process boils down to a simple, logical sequence: screen, diagnose, treat, and monitor. It's the best way to ensure every piece of the puzzle is accounted for before and during your therapy.
The First Step: Screening for OSA Risk
Before a single prescription is written, a good clinician will start with a thorough evaluation for Obstructive Sleep Apnea (OSA) risk. This initial check is usually quick, completely non-invasive, and can be done right in the office.
The go-to tool for this is the STOP-BANG questionnaire. It's a straightforward, eight-question survey that looks at the biggest risk factors: Snoring, Tiredness, Observed apneas, high blood Pressure, Body Mass Index (BMI), Age, Neck circumference, and Gender. A high score doesn't mean you have sleep apnea, but it's a major red flag that tells us we need to dig a little deeper.
It's like running a diagnostic check before a major software update. You wouldn't install powerful new code without scanning for viruses first, right? In the same way, we don't want to introduce a powerful hormone like testosterone without making sure an underlying issue like OSA won't cause system-wide problems.
Getting a Formal Diagnosis: The Sleep Study
If that initial screening raises any red flags, the next step is a formal sleep study, also known as polysomnography. This is the definitive way to diagnose sleep apnea and figure out how severe it is.
You've generally got two options here:
- At-Home Sleep Apnea Test (HSAT): This is the convenient choice for many. You get a simple device to wear overnight in the comfort of your own bed, which tracks key metrics like your breathing patterns, blood oxygen levels, and heart rate.
- In-Lab Sleep Study: This is the deep-dive option, done at a specialized sleep center. A technician monitors everything from brain waves and eye movements to muscle activity, giving your doctor a complete, highly detailed picture of what’s happening while you sleep.
Your doctor will help you decide which test makes the most sense for you based on your health history and screening results.
The Clinical Pathway for Safe Management
Once all the data is in, your healthcare provider can build a clear plan to manage both conditions without compromising your health. The goal is simple: create a stable foundation so TRT can do its job properly.
Here's the standard, four-step approach we follow:
- Screen Before Starting: Every man considering TRT should be screened for OSA risk with a tool like the STOP-BANG questionnaire. No exceptions.
- Diagnose If Necessary: If the screening suggests a moderate to high risk, a formal sleep study is ordered to get a definitive diagnosis.
- Treat OSA First: If OSA is confirmed, treatment needs to start right away. The most effective and common treatment is Continuous Positive Airway Pressure (CPAP) therapy. Many responsible clinicians will require you to be using your CPAP consistently before or at the very same time you begin TRT.
- Monitor Continuously: After starting TRT, we keep a close eye out for any new or worsening OSA symptoms. This allows us to catch any changes early and adjust the plan as needed.
This decision guide helps illustrate the process and highlights how symptoms of low T and sleep apnea can often overlap.
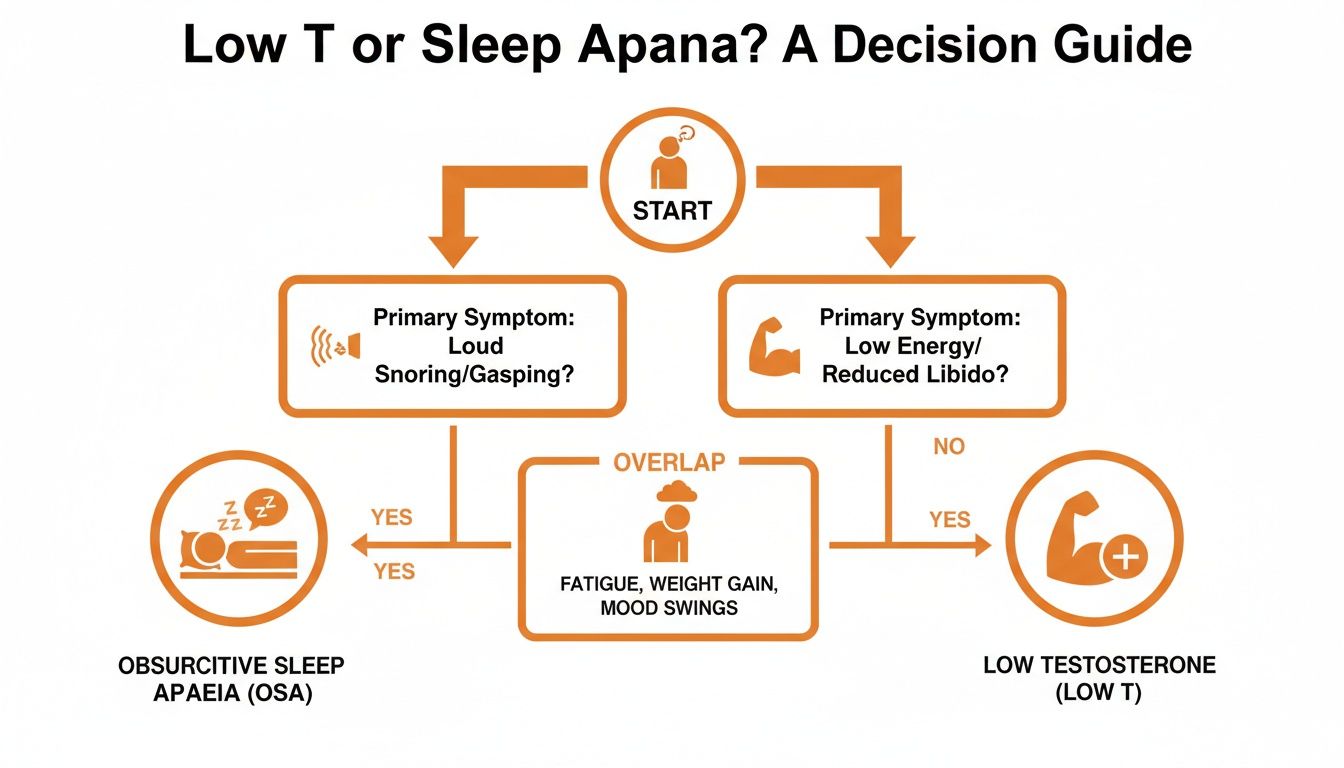
As you can see, shared symptoms like fatigue can point to either condition, which is exactly why proper medical screening is so critical to figure out the real root cause.
By treating sleep apnea first, you’re not just eliminating a major health risk—you might actually give your natural testosterone production a boost. When your body finally gets the restorative sleep it needs, it starts functioning better, which can make TRT more effective at lower, safer doses.
This proactive strategy is grounded in solid research. We know from studies that men with severe OSA often have shockingly low testosterone levels. We also know that screening for OSA before TRT helps prevent other complications, like polycythemia (a risky spike in red blood cells), ensuring you get all the benefits of therapy without the avoidable risks.
Ultimately, this careful, step-by-step approach turns the relationship between testosterone and sleep apnea from a potential problem into a well-managed partnership for your health. If you're ready to move forward, our guide explains how to start hormone replacement therapy with safety as the number one priority.
Answering Your Questions About TRT and Sleep Apnea
When you're trying to figure out the connection between testosterone and sleep apnea, a lot of questions pop up. It's a tricky area of men's health, with symptoms that can easily overlap and treatment decisions that need to be made carefully.
Let's dive into some of the most common questions guys have when discussing Testosterone Replacement Therapy (TRT) and its link to obstructive sleep apnea (OSA). The goal here is to give you direct, clear answers so you can feel confident about your health choices.
If I Treat My Sleep Apnea, Will My Testosterone Return to Normal?
This is a great question, and it gets right to the point. For many men, the answer is a big, encouraging yes. Treating sleep apnea, typically with CPAP therapy, often leads to a significant and very real increase in the body's own natural testosterone production.
Here’s a way to think about it: your body's hormone-making machinery has been running with the brakes on, sabotaged by nightly oxygen drops and terrible sleep. When you start CPAP, you're finally taking the brakes off. You're giving your system the two critical things it needs to run properly: stable oxygen and deep, restorative sleep.
This simple act of restoring order gives your endocrine system the green light to get back to work. It’s not uncommon for men to see their testosterone levels climb back into a healthy range after just a few months of using their CPAP machine every night.
That said, it's important to have realistic expectations. While CPAP is a game-changer for boosting natural T, it isn’t a magic bullet for every single person. The final result really depends on a few key factors.
Here’s what you need to consider:
- Your Starting Point: If your testosterone was just borderline low because of bad sleep, CPAP might be all you need to get back in the game. But if your levels were already in the tank, CPAP will help, but it might only bring them up part of the way.
- Age and Overall Health: Age is a huge factor in natural testosterone production. Other health issues can also put a ceiling on how much of a rebound you'll see.
- Severity of the Apnea: The worse the sleep apnea was, the more it was likely suppressing your hormones. This means that treating severe apnea can sometimes lead to more dramatic improvements in T levels.
The best approach is simple and methodical. First, get serious about treating the sleep apnea. That means using your CPAP every single night, without fail. Then, after about three to six months of consistent use, go get your hormone levels checked again. This gives you and your doctor a clear picture of how much your natural production has recovered and helps you decide if TRT is still the right next step.
I Am on TRT and Think I Have Sleep Apnea. What Should I Do?
If you're already on TRT and start noticing the classic signs of sleep apnea—maybe your partner is complaining about your snoring, you wake up gasping for air, or you feel wiped out all day—you need to take action right away.
Your first move is to call the doctor who prescribes your TRT. Whatever you do, don't stop your therapy on your own. Stopping TRT cold turkey can trigger a whole new set of nasty side effects and throw your hormones completely out of whack. Your doctor needs to be involved to guide you safely.
They will almost certainly recommend a sleep study to find out what's going on. It’s the only way to know for sure if you have OSA and to figure out how severe it is. Once you have those results, you can build a solid plan.
In this situation, the goal is almost never to stop testosterone therapy. Instead, the focus shifts to treating the sleep apnea, usually with a CPAP machine. By managing both conditions at the same time, you get the best of both worlds. In fact, treating the OSA will make your TRT safer and more effective, while dramatically lowering the cardiovascular risks that come with untreated sleep apnea.
Are There Natural Ways to Improve Both Conditions?
Absolutely. While medical treatments like CPAP and TRT are incredibly effective, your daily habits form the foundation for good health and can have a massive impact on both testosterone and sleep apnea. Think of these as strategies that work hand-in-hand with your medical treatments to get the best possible results.
Without a doubt, the single most powerful natural strategy is weight management. Excess body fat—especially the visceral fat around your midsection and neck—is a primary driver of both low T and sleep apnea. Fat tissue contains an enzyme that converts your precious testosterone into estrogen, actively lowering your T levels. At the same time, that extra weight around your neck literally squeezes your airway, making it much more likely to collapse when you sleep.
Here are the lifestyle changes that will give you the most bang for your buck:
- Nail Your Nutrition and Exercise: A diet built around whole foods, combined with a smart exercise routine, is your best weapon. That means a mix of resistance training to build muscle (which boosts metabolism and supports hormones) and cardio for fat loss and heart health.
- Cut Back on Alcohol: This is especially important in the evening. Alcohol is a muscle relaxant, and when you drink it before bed, it can cause the tissues in your throat to go limp, worsening airway collapse and making apneas more frequent and severe.
- Master Your Sleep Hygiene: While good habits won't cure a diagnosed case of OSA, they can improve your overall sleep quality. This means keeping a consistent sleep schedule, making sure your bedroom is dark and cool, and putting away screens an hour before bed.
Think of your lifestyle as the foundation of a house. TRT and CPAP are the strong walls and roof. You need both to build something that's safe, solid, and will last for years to come.
At Elite Bioscience, we believe in looking at the big picture of men's health, always putting safety and real-world results first. If you're ready to see how hormone optimization can fit into your overall wellness strategy, a great place to start is by exploring our personalized therapy options.
QUICK SEARCH
Make an account today to start your journey towards a better and healthier lifestyle.



